Food Allergies vs. Food Intolerance: How They Really Affect Eczema and Your Skin Health
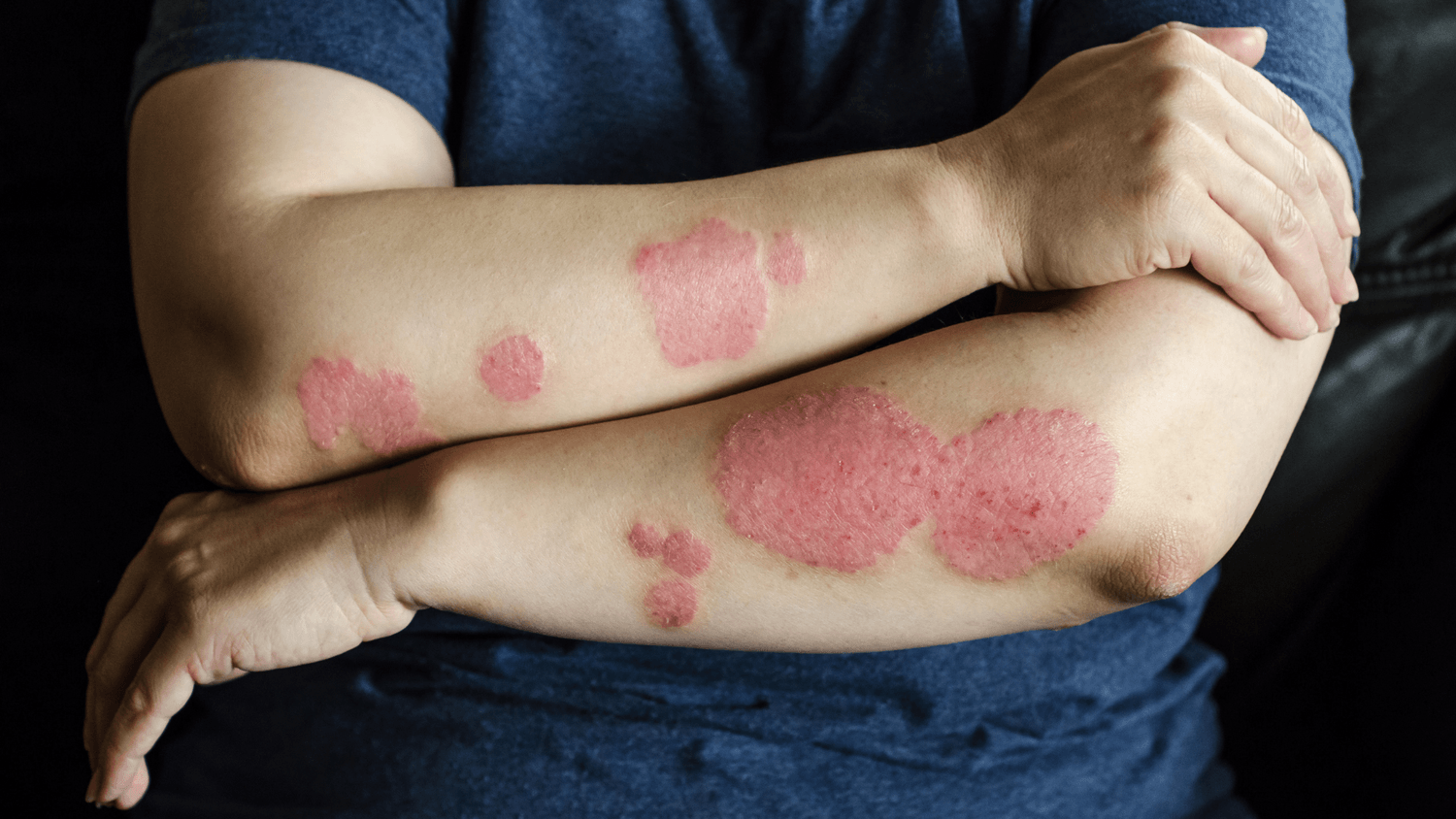
If you have eczema, you know how unpredictable it can be. One day your skin is calm, the next it’s inflamed and itchy, and sometimes it’s hard to figure out why. Naturally, many people wonder: “Could it be something I ate?”
Food can indeed influence eczema, but it’s rarely the whole story. Eczema is a complex condition influenced by genetics, immune system activity, skin barrier health, and environmental triggers. Food is just one piece of the puzzle — but an important piece, especially when it comes to identifying personal triggers safely.
Before trying elimination diets or guessing what to avoid, it’s essential to understand the difference between food allergies and food intolerances, because the body reacts very differently to each.
If you have eczema, you know how unpredictable it can be. One day your skin is calm, the next it’s inflamed and itchy, and sometimes it’s hard to figure out why. Naturally, many people wonder: “Could it be something I ate?”
Food can indeed influence eczema, but it’s rarely the whole story. Eczema is a complex condition influenced by genetics, immune system activity, skin barrier health, and environmental triggers. Food is just one piece of the puzzle — but an important piece, especially when it comes to identifying personal triggers safely.
Before trying elimination diets or guessing what to avoid, it’s essential to understand the difference between food allergies and food intolerances, because the body reacts very differently to each.
Food Allergies: When Your Immune System Overreacts
Eggs
Cow’s milk
Peanuts and tree nuts
Soy
Wheat
Symptoms of a Food Allergy
Hives or raised red bumps
Swelling of lips, tongue, or throat
Difficulty breathing or wheezing
Sudden eczema flare-ups in sensitive individuals

⚠️ Important: Severe allergic reactions, such as difficulty breathing, can be life-threatening. If you suspect a serious allergy, consult an allergist immediately.
Food Intolerances: Subtle, Delayed Reactions
Unlike allergies, a food intolerance does not involve an immune attack. Instead, the body may struggle to digest, metabolize, or tolerate certain foods. Reactions are often delayed, subtle, and cumulative, which can make it harder to pinpoint the trigger.

Common Food Intolerances in Eczema
Dairy products (especially lactose or milk protein)
Wheat or gluten
Fermented foods
Additives, preservatives, and artificial coloring
Symptoms of Food Intolerance
Digestive discomfort (bloating, gas, diarrhea)
Gradual worsening of eczema over hours or days
Fatigue, headaches, or brain fog
Even though these reactions are generally less severe than allergies, they can trigger systemic inflammation, subtly aggravating eczema and making flare-ups more frequent or intense.
Food Isn’t the Whole Story
It’s easy to assume that food is the main culprit behind every flare-up, but most eczema episodes are not solely food-related. Genetics, skin barrier dysfunction, immune overactivity, and environmental factors usually play a bigger role.
Extreme or unnecessary dietary restrictions can sometimes cause nutritional deficiencies, stress, or frustration, especially in children. Instead, the goal is to identify the specific foods that affect your skin in a safe and structured way.
Tracking Your Triggers: A Safe and Practical Approach
Identifying what triggers your eczema can feel overwhelming. Reactions may be delayed, subtle, or cumulative. This is where tracking and observation become invaluable.
One of the most effective tools for this is the Gentle Reset Journal. It’s designed to help you:
Record meals, snacks, and beverages along with your skin condition
Track flare-ups, sleep, and stress levels
Notice patterns and identify personal triggers without guesswork
Build daily habits that support anti-inflammatory skin health
By using the journal alongside the strategies below, you can turn guesswork into clarity and start making informed choices for your skin.
Steps to Identify Triggers Safely
1. Keep a Detailed Journal
Track meals, symptoms, and lifestyle factors like sleep, stress, and exercise
Look for patterns over weeks, not just single meals
2. Work With Professionals
Allergists can confirm true food allergies
Dietitians can guide elimination diets safely and ensure nutritional balance
3. Use Careful Elimination and Reintroduction
Remove suspected triggers for 2–4 weeks
Reintroduce one food at a time while monitoring skin, digestion, and energy levels
4. Focus on Anti-Inflammatory Foods
Fatty fish, leafy greens, berries, turmeric, and healthy fats reduce systemic inflammation
Minimize processed foods, refined sugars, and inflammatory fats
The Bigger Picture: Multi-Factorial Flare-Ups
Even with careful tracking, food is only one part of managing eczema. Other key contributors include:
Skin barrier dysfunction – compromised skin is more sensitive to irritants
Immune system activity – overactive immune responses can worsen eczema
Environmental triggers – allergens, chemicals, plastics, and climate changes
Lifestyle factors – stress, sleep quality, and daily habits
By combining tracking, professional guidance, anti-inflammatory habits, and environmental awareness, you can gain a more complete understanding of your eczema and reduce flare-ups safely.
Key Takeaways
Food allergies involve the immune system and can cause immediate, severe reactions.
Food intolerances are delayed reactions that may subtly worsen eczema over time.
Most eczema flare-ups are multi-factorial, not just food-related.
Tools like the Gentle Reset Journal make tracking triggers easy, helping you make informed choices for long-term skin health.
Combining professional guidance with anti-inflammatory habits and consistent observation empowers you to manage eczema with confidence.
Understanding your body’s unique responses can transform how you approach eczema — moving from confusion and frustration to clarity, control, and calmer, healthier skin.
Download your Gentle Reset Journal: https://www.theantiinflammatorymindset.com/the-gentle-reset-journal
Sources:
1. National Eczema Association — Food and Eczema
2. American Academy of Allergy, Asthma & Immunology — Food Allergies vs. Food Intolerance
3. Mayo Clinic — Food Allergy vs Food Intolerance: What's the difference?
4. National Library of Medicine — The Role of Food Allergy in Atopic Dermatitis
Get in touch
Feel free to get in touch with us via email: support@theantiinflammatorymindset.com
TAIM | Privacy Policy | Terms and Conditions




